National annual report on drug issues
Annual report sent to the EMCDDA (European Monitoring Centre for Drugs and Drug Addiction) giving an overview of the latest developments on the drug problem in France.
Cliquez ici si vous souhaitez télécharger les rapports nationaux disponibles en français 
2022 report
The 2022 report is divided in 10 workbooks: Drug Policy, Legal Framework, Drugs, Prevention, Treatment, Best Practice, Harms and Harm Reduction, Drug Market and Crime, Prison and Research.
Drug policy
The 2018-2022 National Plan for Mobilisation against Addictions, which was introduced by the government in December 2018, promotes an approach targeting all psychoactive substances (alcohol, tobacco, illegal drugs) and other forms of addictive behaviours (gambling, doping).
The 2018-2022 Plan has a clear and assertive discourse on the risks and harms associated with addictive behaviour. The government strategy focuses on prevention, vulnerable groups and health inequalities. The 2018-2022 National Plan for Mobilisation against Addictions pays special attention to the quality of responses to the consequences of addiction for both individuals and society. On the aspects relating to narcotics and security, the Plan shows a strong commitment to combating trafficking in order to respond to the challenges posed by the increase in supply and the direct consequences of trafficking (insecurity, violence, parallel social organisation in certain areas of the country, weakening of the legal economy, etc.). The Plan strengthens the interministerial dimension of public action in the field of addictions by proposing reinforced steering of support for research. With regard to the implementation of the national guidelines in the French regions and departments, the 2018-2022 Plan emphasises its desire to unite the action of State services, local authorities and civil society and authorises regional prefects to set up roadmaps for their region. The development of the 2018-2022 Plan was guided by the principle of strengthening the coherence of public action over the period of implementation of its measures and the search for their articulation with other government strategic programmes (prevention, health, road safety, child poverty, students, detained persons, housing, overseas territories).
The 2018-2022 National Plan for Mobilisation against Addictions was recently evaluated as part of an internal evaluation process, led by the Interministerial Mission for Combating Drugs and Addictive Behaviours (MILDECA). The evaluation had a dual purpose: to establish an assessment of territorial dynamics and to design operational proposals that will support the next government strategy. The methodological approach, which was qualitative in nature, was based on work and exchanges with State services involved in the fight against drugs and addictive behaviours, in two regions that are representative of the territorial dynamics underway: Occitanie and Normandy. Regional and departmental prefectures, regional health agencies, public prosecutors and education authorities were also involved. This evaluation exercise was reinforced by additional insights provided by the plan's indicator monitoring table.
The directions of public policy in the field of drugs and addictions are defined by the "Interministerial Committee for Combatting Drugs and Addictive Behaviours", under the authority of the Prime Minister. Prior to this stage, MILDECA is responsible for drafting the decisions of the interministerial committee, then coordinating French government policy for combatting drugs and preventing addictive behaviours, and for ensuring that the decisions of the interministerial committee are implemented. On the authority of the Prime Minister, its scope of action includes prevention, treatment, harm reduction measures, integration, trafficking, law enforcement and research, monitoring and training of staff involved in activities to reduce supply and demand. A network of approximately 101 territorial representatives (generally the senior local government officers’ general administrators of the “département” or “region”) on a national scale guarantees the consistency of the implemented actions. Since 1st January 2020, the Anti-Narcotics Office (OFAST) - a service attached to the General Directorate of the National Police (DGPN) - has been designated as the lead agency for the internal security forces, Customs officers and the national navy, as well as the judicial authority in the fight against trafficking. The service brings together officers from the police, gendarmerie and Customs, as well as liaison officers. At the territorial level, 103 operational drug intelligence units (CROSS) carry out essential work in collating information for the purposes of knowledge of trafficking, action and prosecution.
The social cost of drugs in France was estimated at three points, in 1996, 2003 and 2010. For the year 2010, the latest estimate published by the French Monitoring Centre for Drugs and Drug Addiction (OFDT) in September 2015 evaluates this cost at 8.7 billion euros for illegal drugs, far from the amount estimated for alcohol (118 billion) and for tobacco (122 billion). A new estimate of the social cost of drugs is being carried out under the coordination of the OFDT, financed by the Addiction Fund. A new update (2021 data) will be published shortly.
In 2020, total public spending on the fight against drugs and addictive behaviour is estimated at 2.31 billion euros. The contribution from the State and Health Insurance represents 0.13% of the gross domestic product (GDP) (Eurostat 2022), with 44% of the total for demand reduction initiatives, 54% for supply reduction activities and almost 2% of the resources allocated to cross-country activities (coordination and international cooperation).
Two important topics marked the period of 2021-2022: the French Presidency of the Horizontal Drugs Group and the latest developments regarding drug consumption rooms.
As part of the French Presidency of the Council of the European Union, MILDECA chaired the Horizontal Drugs Group. The central themes targeted by France were the review of the European Monitoring Centre for Drugs and Drug Addiction’s mandate, the European Union's response to the increase in the supply of and demand for cocaine, taking into account the environmental impact of the production, transport and use of drugs, and the relationship between drugs and digital technology.
With regard to harm reduction policy, the Social Security Financing Act for 2022, in light of the positive results of the evaluation conducted by Inserm in particular, has extended for an additional three years the experimentation with the system of drug consumption rooms renamed Haltes Soins Addictions (HSA).
![]() Download Workbook 1 : Drug Policy
Download Workbook 1 : Drug Policy
Legal framework
In France, the regime applicable to acts of drug use and trafficking was established by Law no 70-1320 of 31 December 1970 on health measures to fight drug addiction and combat the trafficking and use of poisonous substances. The provisions of this law were since codified in the French Public Health Code (CSP in French).
The penalties incurred by the perpetrators of drug-related offences depend on the severity of the offences committed (see T1.1.1), thus the illicit use of drugs (Art. L.3421-1 of the Public Health Code) is less severely punished than drug trafficking (Art. 222-34 et seq. of the Penal Code) or related offences (money laundering, failure to provide proof of resources corresponding to one's lifestyle, etc.), because the perpetrator is considered by the law to be a delinquent as well as a patient. The criminalisation of drug use is reflected in a wide range of responses: some suspend or cancel prosecution but are still sanctions, such as alternatives to prosecution or fixed penalty notices; others result in legal proceedings, which may lead to a fine or other types of sentence (or even, sometimes, imprisonment).
Although French law makes no distinction between products as some countries do, it distinguishes between the illicit sale and supply of narcotics to a person in light of their personal use and other situations. Repeat offences are more severely sanctioned (see T1.1.2).
There are no specific laws regulating new psychoactive substances (NPS). The rationale for classifying a NPS on the list of narcotics is both individual (each prohibited substance is named on the list) and generic (See T1.1.3).
![]() Download Workbook 2 : Legal framework
Download Workbook 2 : Legal framework
Drugs
Drug use, polydrug use and the main illicit drugs
The latest available data in terms of levels of illicit drug use in France come from the 2020 Health Barometer Survey of Santé publique France for cannabis and from the 2017 Health Barometer Survey for the other illicit drugs. In 2020, cannabis is still by far the most widely used illicit substance, both among teenagers and the adult population (46% of 18 to 64-year-olds), with overall 18 million people having already tried it. The overall proportion of current users (in the last year) is 11.3% among adults.
Among last year users aged 18 to 64 years (11%), according to the 2017 Health Barometer Survey, the proportion of those at high risk of problem cannabis use (according to the Cannabis Abuse Screening Test, CAST – see details in T1.2.3 of the 2016 ‘Drugs’ workbook) is 25%, i.e. 2.3% of the French population aged 18 to 64 years in 2017. Cannabis is also the most frequently reported substance mentioned as the principal reason for entering drug treatment (CSAPA). As far as synthetic cannabinoids are concerned, 1.3% of adults aged 18 to 64 state that they have already used such substances. Their use levels are similar to heroin or amphetamines.
Cannabis use among adults aged 18 to 64 stabilised between 2017 and 2020, at a high level, irrespective of age groups and frequency of use: this trend is part of the dynamic context of supply in France, particularly with the local production of herbal cannabis (industrial plantations but also personal cultivation), alongside the innovation and diversification of the resin market (See T.2.1 of the 2021 ‘Market & Crime’ workbook).
In 2017, cannabis is also the illicit substance most widely used between the ages of 11 and 16 years, particularly among boys. (See T0.1 of the 2021 ‘Market & Crime’ workbook)
The last ESCAPAD survey of 17-year-olds was conducted in 2022. The results will be available at the end of 2023.
In the survey on representations, opinions and perceptions regarding psychoactive drugs (EROPP) conducted at the end of 2018 among people aged 18 to 75, nearly 9 out of 10 respondents (88%) spontaneously reported cannabis as a "drug" they know, even if only by name (See T4.1 of the Cannabis section for more on opinions).
In 2017, the spread of cocaine, the second most widely consumed illegal substance, is considerably lower: almost ten times fewer people had already tried it. The same applies to MDMA/ecstasy (See T0.1 of the 2021 ‘Market & Crime’ workbook for more on uses among the adult population).
The latest ENa-CAARUD survey carried out at the end of 2019 at the CAARUD low-threshold structures (Support Centre for the Reduction of Drug-related Harms) confirmed the qualitative observations of the TREND scheme, which showed a shift in the consumption of the most precarious users towards the cheapest products, medicines and crack cocaine when it is available. It should also be noted that there has been a clear increase in poverty and social insecurity among users, as well as a significant increase in the prevalence of people who have used cocaine in the last 30 days (from 50% to 69% from 2015 to 2019), based in particular on cocaine.
The use of illicit drugs with alcohol, tobacco and prescription drugs
In both the French Public Health Agency’s health barometer (adult population) and the OFDT’s ESCAPAD survey (17-year-olds), polydrug use is defined as using at least two of the three following substances over the period of a month: alcohol, tobacco and cannabis. These are not necessarily concurrent uses. (See T0.2 of the 2021 ‘Market & Crime’ workbook)
The last ESCAPAD survey of 17-year-olds was conducted in 2022. The results will be available at the end of 2023.
Regarding the public received in Youth Addiction Outpatient Clinics (CJC), please read T0.2 of the 2021 ‘Drugs’ workbook.
Prevention
Policy and organisation
In France, the addictive behaviour prevention policy refer to licit (alcohol, tobacco and psychotropic medicines) and illicit psychoactive substances, but also to other forms of addiction (gambling, gaming). Under the State responsibility, this strategy is coordinated at central level by the Interministerial Mission for Combating Drugs and Addictive Behaviours (MILDECA) and implemented at local levels by deconcentrated services. General goals are not only to delay if not to prevent the onset of use, but also to curb addictive practices and the related abuses and risks. The 2018-2022 National Plan for Mobilisation against Addictions emphasises the implementation of evidence-based approaches, particularly those focusing on psychosocial skills for children and adolescents, and on the early detection of addictive behaviours so that people in need can be guided more effectively to specialised support services.
In the prefectures, the MILDECA project managers outline, within the framework of regional roadmaps, their objectives to prevent addictive behaviour and share them with the State's territorial departments. They dedicate funding to prevention activities granted by the Finance Act and appropriated to them by the MILDECA as well as funding from the Interministerial Fund for Crime Prevention (FIPD). The intervention funding from the Regional Health Agencies (ARS), particularly the Regional Intervention Fund (FIR), and now the Fund for Combatting Addiction to Psychoactive Substances, constitute other sources of financing prevention.
At local level, school prevention activities are implemented by a range of professionals. Prevention in schools relies, in particular, on programmes to strengthen the individual and social skills of pupils (from nursery to secondary school) in order to resist the desire to use drugs, peer pressure and the supply of psychoactive substances.
Prevention interventions
In France, environmental strategies to reduce alcohol and tobacco consumption are well established and enjoy strong political support. School-based universal prevention (including those in agricultural education) and indicated prevention through the Youth Addiction Outpatient Clinics (CJC) which deliver ‘early intervention’ towards young users and their families (in 550 consultation points throughout France) are two pillars of the public responses. Major efforts have been made to develop collective prevention measures in the workplace as well (private compagnies and public services) beyond the remit of occupational physicians as well as in universities through health services and student liaison officers on health. However, preventive responses were enhanced towards priority publics, like youth in deprived urban areas, youth in the care of the judicial youth protection and child welfare services. National media social marketing campaigns against alcohol or tobacco consumption are regularly broadcast, but these are less frequent on the subject of drugs. Two campaigns on cannabis were organised in 2022.
Trends & Quality assurance
During the 2010s, professionals and policymakers are showing increasing interest in the quality of prevention services and programmes offered and how to improve them. Special efforts are being made to extend versions adapted to the French context of the Unplugged and GBG [Good Behaviour Game] programme to primary school classes, as part of a cross initiative between professional organisations and decision-makers. Prevention stakeholders are encouraged but free to refer to guidelines on drug prevention in school or other settings. The ASPIRE grid (Assessment and selection of prevention programmes arising from "EDPQS" quality standard overview) the French adaptation of the EDPQS, remains relatively unknown and appears to not be used very frequently. Since the end of September 2018, a directory of effective or promising prevention interventions that promote health « Répertoire des interventions efficaces ou prometteuses en prévention et promotion de la santé », managed by the French Public Health Agency (SpF-Santé publique France), has been available and is still being expanded.
New development
The 2018-2022 National Plan for Mobilisation against Addictions involves numerous new objectives in terms of prevention in the coming years.
![]() Download Workbook 4 : Prevention
Download Workbook 4 : Prevention
Treatment
National profile
One of the priorities of the 2018-2022 National Plan for Mobilisation against Addictions (MILDECA 2018) is the construction of a health care pathway based on a consolidated primary care and a better structured specialised offer. This priority is broken down into 6 objectives (see T1.1).
The provision of care for drug users is based on the three sectors of the French health system: the primary care sector, the medico-social sector and the hospital sector (see T1.2).
Addiction treatment services
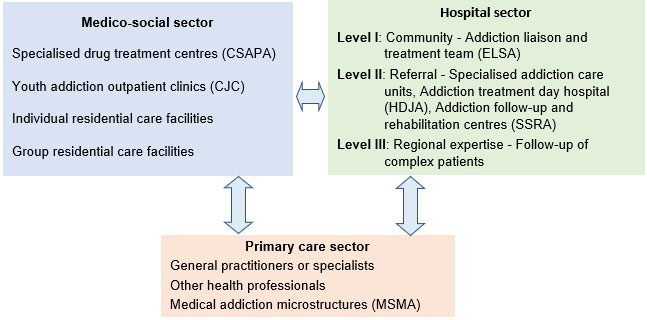
This offer is multidisciplinary and includes the following types of treament:
- Medicinal treatment: substitution or withdrawal and post-withdrawal
- Treatment for psychiatric and somatic comorbidities
- A psychotherapeutic approach
- Socio-educational care
- Harm reduction
- A specific service for the parents or partner of subjects at risk of addiction or who have become addicted (family approach)
The French RECAP scheme underwent a methodological review in 2021-2022. The RECAP data used to produce the TDI data will now be used with a 2-year delay. This will eventually allow statistics to be provided by a larger number of care facilities than has been the case to date. The production of 2021 data will therefore only be available next year. As a result, this WB includes the RECAP 2020 data used in the previous year's report. In the absence of 2021 data, the total number of people starting treatment in specialised drug treatment centres (CSAPA) could be estimated at about 66 000 personnes (see Workbook Treatment 2021), down slightly from 2019. Furthermore, a total of 22 900 patients were dispensed opioid substitution medications in a CSAPA setting in 2019.
The activity of community doctors in the field of addiction treatment mainly involves prescribing opioid substitution medications. According to the latest data from 2018, 161 400 people had a prescription for opioid substitution drugs in France (see Workbook Treatment 2021).
Trends
The number of all users entering treatment (in constant terms) is falling in 2020: the drop is almost 22% overall, and 26% where cannabis is concerned, 16% for opioids and 20% for cocaine (Workbook Treatment 2021).
![]() Download Workbook 5 : Treatment
Download Workbook 5 : Treatment
Best practice
The national action plan on addiction for the 2018-2022 period reaffirms the government’s willingness to reinforce quality in public responses on the basis of observation, research, evaluation and a reinforced training strategy, with a special impetus on prevention. Under the prevention, care and research strategical pillars, it defines quality assurance objectives with regards to the promotion and the implementation of evidence-based knowledge, evaluation and skill raising through training and scientific mediation.
In France, quality assurance in Drug Demand Reduction (prevention, risk reduction, treatment and rehabilitation) builds on specific advocacy, guidelines or trainings from public health institutions or professional societies. It is in the remits of the French Public Health Agency (Santé publique France - SpF) and the French National Authority for Health (Haute autorité de santé - HAS). SpF disseminates evidence in drug prevention research and supports the local experimental transfer of international evidenced-base programmes like Unplugged (Lecrique 2019), GBG, SFP, etc. The HAS diffuses professional guidelines/recommendations on risk reduction and treatment addressing: (i) Opioid Substitution Treatment, (ii) Early intervention and risk/harm reduction for crack or free base users, (iii) Clinics for young drug users, (iv) Treatment of cocaine users, (v) Harm and risk reduction in low threshold services (CAARUD) and lastly (vi) Prevention and harm reduction delivered by drug treatment centres (CSAPA) (released in December 2019).
The two later guidelines (v and vi) serve as a baseline for compulsory evaluations of drug services but the fulfilment of the other guidelines is not a formal prerequisite for support or subsidies. Some tools exist to help decision makers to select quality prevention programmes (EDPQS materials and the ASPIRE toolkit adapted from them) and practitioners to develop quality programmes but the extent to which they are used is unknown.
Professional federations are also engaged in developing quality and professional supports: the portal on addictions for primary care professionals (GPs, school nurses, dentists, pharmacists, midwives, emergency doctors) is an example: https://intervenir-addictions.fr/. This portal was created by the Fédération Addiction with support from the public authorities, the French Public Health Agency (Santé publique France), the OFDT and various other partners in the field of addiction.
The addiction treatment services (so-called CSAPA) are marginally impacted by the existing accreditation and certification systems applied to health establishments and processed by the HAS (French National Authority for Health). However, the CSAPA, most of which were authorised as medico-social establishments at the beginning of the 2010s for a period of 15 years, are required to provide two external evaluations during this period. These evaluations must be carried out by a body approved by the HAS and follow a set of specifications outlined by decree.
Despite a lack of resource services in prevention engineering at local level, there is a noticeable willing at national level to enhance quality in the programmes and services delivered, especially in prevention.
There is a one-year specialised training in addiction in the third cycle of medical studies. Continuing education programmes for medical doctors and other professional in the field of addiction are also in place.
An important dynamic has been engaged to support the extension of evidence-based programmes to develop psychosocial skills, with particular support from the French Public Health Agency (Lamboy et al. 2022). A special impetus has been made to develop the Unplugged programme in France: ten of the thirteen French regions are engaged the implementation of the programme in a limited number of secondary schools. They take part in the elaboration of a national strategy for the adaptation and dissemination of Unplugged, following adaptations to the national context. Many guidelines were issued during the covid-19 epidemic to support help services to continue their activities on the basis of dematerialised means.
![]() Download Workbook 6 : Best practice
Download Workbook 6 : Best practice
Harms and Harm Reduction
National profile and trends harms
The most recent data from the National registry of causes of death (CépiDc) are from 2017 with 417 deaths. This number is probably underestimated.
In 2020, the specific DRAMES register reported 567 deaths related to the misuse of psychoactive substances (503 in 2019) and the specific DTA register recorded 117 deaths related to the use of analgesic drugs (145 in 2019).
Around 19 300 hospital emergency presentations related to drug use were reported in France in 2019 (Oscour® network). These presentations were related notably to cannabis use (29%), opioid use (26%) and cocaine use (12%). Between 2015 and 2019 there was an increase in the proportion of emergency presentations related to cocaine use (12% vs 7%).
Injecting drug use was rarely identified as a mode of infection for people who discovered their HIV status in 2020 (1.5%). At the time of discovery of HIV status, 5% of intravenous drug users were co-infected with hepatitis B virus (HBsAg) and 57% were positive for HCV antibodies.
National profile and trends harm reduction
Harm reduction policy for drug users aims to prevent infections and fatal overdoses linked to substance use and to promote access to care and social rights for drug users. It calls on local actors and relies on:
- A government roadmap for the prevention and treatment of opioid overdose, which includes a naloxone dissemination programme: ready-to-use naloxone kits are available in health care institutions, specialised addiction treatment facilities and in pharmacies.
- A programme for the distribution of prevention materials based on a local offer (CSAPA and CAARUD, pharmacies, automatic distribution machines) and a postal needle exchange programme. The latter makes it possible to improve accessibility by removing obstacles related to geographical distance, opening hours and confidentiality.
- Opioid substitution treatments available in cities, in CSAPAs and in prison.
- National HIV and hepatitis prevention strategies: the actions implemented as part of these strategies focus in particular on strengthening community-based screening and rapid access to treatment and are in line with the objective of eliminating HIV by 2030 and HCV by 2025.
- The drug consumption rooms (DCR) known as “salles de consommation à moindre risque” (SCMR) have become the “Halte soins addiction” centres (HSA). (See T3 and drug analysis as a harm reduction tool in T.1.5.3)..
New developments
Since September 2021, naloxone has again been available in France as a nasal spray: Nixoid® nasal spray 1.8 mg/0.1 ml. It is added to the Prenoxad® intramuscular injection 0.91 mg/ml kit already available on the market. Nixoid® is subject to mandatory medical prescription.
The DCR experiment started in 2016 in Paris and Strasbourg for a period of six years has been extended until December 2025 to allow these harm reduction facilities to be opened in new areas. DCRs are evolving into “Halte soins addiction” (HSA) centres. The HSAs are spaces for harm reduction through supervised use and orientation towards a physical and psychological health pathway adapted to the situation of drug users. They can take the form of mobile units and can also be located in specialised medical and social facilities (CSAPA and CAARUD).
The regulatory scheme for funding and authorising the performance of rapid diagnostic test (RDT) by non-medical staff, which until now has only covered HIV and HCV, was extended to cover HBV in June 2021 (order of 16 June 2021 setting out the conditions for performing RDTs).
With regard to OSTs, the range of opioid substitution drugs was expanded with the launch of Buvidal® in July 2021: a sustained-release injectable solution of buprenorphine, administered on a weekly or monthly basis. Buvidal® is reserved exclusively for professionals in hospitals or CSAPAs. In addition, the National Agency for Medicines and Health Products Safety (ANSM) set up a temporary scientific committee in April 2021 to propose the clinical modalities and conditions for prescribing and dispensing morphine in the treatment of opioid addiction.
In March 2022, the National Authority for Health (HAS) published a recommendation on the proper use of opioid drugs, which aims to reduce cases of overdose and physical addiction to opioids (HAS 2022).
A law to prevent the dangerous and diverted use of nitrous oxide was published in June 2021 (Law no. 2021-695).
![]() Download Workbook 7 : Harms and Harm Reduction
Download Workbook 7 : Harms and Harm Reduction
Drug market and crime
Domestic drug market
Herbal cannabis is the only illegal substance for which production is seen in France. While growing herbal cannabis in metropolitan France was mainly the work of small, self-sufficient growers, the situation began to change at the start of the 2010s with the emergence of cannabis factories run by organised crime groups and with individuals investing in its commercial production.
Given France’s geographic position at the heart of Western Europe, it is a transit area for the main illegal substances (cannabis, cocaine, heroin and synthetic drugs) produced worldwide. This is also the case due to its overseas departments on the American continent (Guadeloupe, Martinique and Guiana) close to the major cocaine production (Colombia, Bolivia, Peru) and transit zones (Venezuela, Brazil, Suriname).
Cannabis resin used in France comes from Morocco and usually transits through Spain while herbal cannabis is imported mainly from Spain, the Netherlands and Belgium.
The cocaine used in France is produced mainly in Colombia. It mainly passes via sea routes through the south via Spain (Algesiras) and the north via the Netherlands (Rotterdam), Belgium (Antwerp) and to a lesser extent Germany (Hamburg). In recent years, cocaine, transiting in particular through Brazil and Venezuela then via the French West Indies, has been entering the European continent through the port of Le Havre. There has also been a major increase in air trafficking by “mules” between Guiana and mainland France since 2011.
The heroin used in France mainly comes from Afghanistan (brown heroin) and passes via the Balkans (Turkey, Greece, Albania). the Netherlands, ahead of Belgium, is the main platform which supplies French dealers.
Synthetic drugs (MDMA/ecstasy, amphetamines) used in France also mainly come from the Netherlands.
National drug law offences
In 2021, the total number of persons accused of narcotic use in France is 189 713 (against 132 046 in 2020). 8 out of 10 people accused of a drug-related offence corresponded to simple use. The number of people involved in trafficking offences in 2021 in mainland France was 17 822, an increase compared to 2020 (14 791), while the number of user-dealers was 16 845 (compared to 14 844 in 2020). In 2010, 90% of the arrests concerned the simple use of cannabis, 5% simple heroin use, and 3% simple cocaine use (since 2010 national statistics no longer provide details of arrests for each substance).
Key drug supply reduction activities
The National Plan for Mobilisation against Addictions (2018-2022) emphasises the importance of implementing a genuine national strategy based on better coordination between the various services involved (police, customs, Gendarmerie, justice). Money laundering, a key issue in a dynamic French drug market, is a major priority. The challenge of international cooperation, in particular, has also been placed at the forefront, notably the important role of French overseas departments (Guiana, Martinique and Guadeloupe, together with the French overseas territory Saint-Martin) in supplying the mainland market with cocaine. France's international actions are mainly based on the networks of internal security attachés, customs attachés and liaison magistrates in the main production and transit countries. Lastly, emphasis is placed on prevention to stop young people, especially minors becoming involved in local trafficking, firmly established in large cities.
In February 2020, the Ministry of the Interior officially announced the creation of OFAST (Anti-Narcotics Office), which succeeds OCRTIS (Central Office for the Repression of Drug-related Offences). This creation corresponds to the State's desire to increase cooperation between the various services in charge of law enforcement: police, customs, military police [gendarmerie] and justice. OFAST is organised into three divisions, "strategy", "intelligence" and "operations", to respond to the three missions "understand", "target" and "act". They are headed respectively by a customs administrator, a military police [gendarmerie] colonel and a divisional commissioner. The deputy head of the office comes from the judiciary. At a territorial level, OFAST has eleven regional offices and five territorial detachments. Since September 30, 2020, 104 operational drug intelligence units (CROSS) have been deployed throughout the country, one per department. One of their missions is to establish a map of the deal points located in French territory and their evolution on a quarterly basis. In 2021, the government announced the creation of a reporting portal for citizens to provide the police and gendarmerie with information about narcotic trafficking and its actors. This information is then transmitted to the CROSS for processing. This scheme should be fully operational during 2022.
In addition, the extent of trafficking in ports and airports has led OFAST and Customs to create CROSS THEMATIQUES covering port, airport and postal activities.
In addition, in order to increase the confiscation of criminal assets linked to drug trafficking, the government decided on 1 January 2021 to strengthen the resources of the Agency for the Recovery and Management of Seized and Confiscated Assets (AGRASC) by opening two regional offices in Lyon and Marseille. In 2022, two more regional branches are being established..
![]() Download Workbook 8 : Drug Market and Crime
Download Workbook 8 : Drug Market and Crime
Prison
With 69 448 inmates, there are 114 inmates for every 100 beds in France. According to data from prisons administration directorate, the prison population in France as of the first of January 2022 consists of 77.5% convicted inmates, with 13.5% of them for a drug-related offence (DLO) or other public health violations.
The only recent surveys on the subject merely provide preliminary or partial data because they are not nationwide. They estimate the proportion of people using cannabis at between 35 and 40%. Quantification of other products leads to very different results depending on the studies. No studies provide data on NPS use in prisons. Inmates have greater rates of infectious disease than the general population: although declining, HIV infection prevalences vary, depending on the source, from 0.6% to 2.0% (three to four times the prevalence in the general population), while prevalences of HCV are from 4.2% to 6.9% (four to five times higher.
Health care in prison is made up of prison health units (USMP) which offer somatic and psychiatric care. Psychiatric care units (regional medico-psychological hospital services - SMPR) coordinate and support USMP. They have hospital psychiatric places for during the day. To treat people presenting with addictive behaviour and the resulting somatic and/or psychiatric symptoms, these units can benefit from working with a CSAPA (specialised drug treatment centre) in a prison environment. A reference CSAPA in charge of helping prepare prisoners for getting out, is designated to each prison.
To guarantee the application of harm reduction measures, two main ways of preventing the spread of infectious diseases have been implemented in prison settings since 1996. Firstly, inmates have to be able to not only continue their opioid substitution treatment (OST) that was prescribed to them before they were imprisoned but to also start such a treatment if they so desire. In addition to substitution, prison establishments offer prevention and decontamination tools for fighting against HIV and hepatitis’s.
Since 2009, different laws have proposed to step up harm reduction measures in prison. The main lines of improvement concern the increased scope and role of the reference CSAPA, routine implementation of screening tests, and widespread access to all existing harm reduction measures, including needle and syringe exchange programmes. These objectives are reasserted in the 2016 health reform law.
New developments
Around 12 900 inmates received opioid substitution treatment in 2018, representing 7% of those who stayed in a prison setting.
Despite the continuation of the COVID epidemic in 2021-22, French prisons have generally returned to their normal functioning. However, the epidemic is monitored and specific measures are taken in the event of an outbreak being observed in an establishment.
A medico-economic evaluation of the URUDs (drug user rehabilitation units) was conducted in 2017 and 2022. It confirmed the results of the OFDT evaluation in 2016, which noted the beneficial effects of the URUD on its residents, recommended that the evaluation be continued and proposed that the system be duplicated in 3 or 4 new establishments.
Research
National profile
In France, the Ministry of National Higher Education, Research and Innovation (MENESR) designs, coordinates and implements national policy on research and innovation. Two primary academic organisations, the National Centre for Scientific Research (CNRS) and the National Institute for Health and Medical Research (INSERM), cover a wide range of research areas, from neurosciences, through public health and clinical research to social sciences.
The French National Focal Point (OFDT) is the main body involved in drug-related data collection, studies and network development. It collaborates extensively with national and European drug-related research teams. Dissemination of data and research results are also part of its mandate, together with publishing in national and international scientific journals, and promoting the use of research results in practice and policymaking.
The Interministerial Mission for Combating Drugs and Addictive Behaviours (MILDECA) is the central structure close to the Prime Minister responsible for coordinating governmental action in the drugs field. Part of its role is to promote and fund drug-related research. Through its interministerial position and its collaboration with the OFDT and other partners, MILDECA plays a major role in the transfer of knowledge to decision-makers, professionals and citizens in France. MILDECA uses its own appropriations (Finance Act/drugs fund) to support research of a particularly strategic nature for steering public policies on drugs and addictive behaviour.
New development
In line with previous government plans, developing research and observation in the field of addictions is key in order to provide information on the implementation of public policies. It represents therefore one of the 6 major challenges included in the 2018-2022 National Action plan on Addictions (MILDECA 2018). The measures to be implemented focus on two main priorities:
1) Bringing science, political policy-making and citizens closer together;
2) Extending knowledge in all areas of public action.
In order to improve links between the scientific community, policymakers and citizens, the plan aims to increase places and times for meetings about spreading knowledge on addiction, both nationally and regionally. The importance of the focal point (OFDT) is underlined as it enjoys ideal positioning for speeding up transfer of knowledge and its appropriation by decision-makers, professionals and citizens.
The plan highlights several key areas where new knowledge is required: prevalence of use among vulnerable groups (people with disabilities, people living in poverty, people subject to a court order, migrants), influence of environmental factors and available preventive and healthcare supplies on the dependence and treatment trajectories, individual vulnerability factors, gender specific factors, etc.
In order to prevent addictive behaviours, emphasis is placed on carrying out intervention research in schools and workplaces. The plan also promotes the development of knowledge related to marketing strategies that influence how the risks of using are perceived among young people. Such information is required in order to deconstruct the discourse conveyed by industrialists and to put in place appropriate responses.
To better reduce risks and improve care and access to care, the plan confirms the need to support clinical and therapeutic research by encouraging a transversal and collaborative approach. Evaluating medico-social and harm reduction interventions is also valued.
Moreover, in terms of questioning the effectiveness of criminal solutions, the authorities stress the need to develop evaluative research in this field in order to encourage solutions to develop the most promising judicial measures. As regards research relating to drug supply, the plan notably encourages improved monitoring of new psychoactive substances and studies on the changes in supply.
![]() Download Workbook 10 : Research
Download Workbook 10 : Research
All reports :
Drugs in Europe
![]() 2023 EMCDDA European Drug Report
2023 EMCDDA European Drug Report
The European Drug Report 2023: Trends and Developments presents the EMCDDA’s latest analysis of the drug situation in Europe. Focusing on illicit drug use, related harms and drug supply, the report contains a comprehensive set of national data across these themes and key harm-reduction interventions. This report is based on information provided to the EMCDDA by the EU Member States, the candidate country Türkiye, and Norway, in an annual reporting process.
The annual Statistical Bulletin contains the most recent available data on the drug situation in Europe provided by the Member States. These datasets underpin the analysis presented in the European Drug Report. All data may be viewed interactively on screen and downloaded in Excel format.
![]() The European Union and the drug phenomenon
The European Union and the drug phenomenon
 The European Union & the drug phenomenon : Frequently asked questions, joint publication between the EMCDDA and the European Commission, october 2010, 12 p.
The European Union & the drug phenomenon : Frequently asked questions, joint publication between the EMCDDA and the European Commission, october 2010, 12 p.



